Session Information
Date: Thursday, June 23, 2016
Session Title: Other
Session Time: 12:00pm-1:30pm
Location: Exhibit Hall located in Hall B, Level 2
Objective: Here we report a case with posttraumatic functional shoulder movement disorder.
Background: Focal posttraumatic shoulder movement disorders are seen rarely. Focal posttraumatic movement disorder is a controversial ill-defined subject. Its etiology encompasses a variety of situations from functional movement disorders to peripherally induced dystonia. Clinical courses, treatment responses are varied.
Methods: A 35 year-old man reported a traumatic shoulder injury which emerged after lifting a barbell 3 years ago. Then he had repetitive movements at his right shoulder. Involuntary movements were brought about while his shoulder was standing still. The examination was normal except irregular forward-backward movements of his right shoulder, which repeated about 30 times per minute. These movements have lasted all day, except during sleep and times he repressed the movements intentionally. No sensory tricks observed and movements were better when he extended his arms forward. Distraction (mental arithmetic, voluntary movements of unrelated parts of the body) decreased the frequency and amplitude of the movements.
Results: All related laboratory were un¬remarkable. Brain magnetic resonance imaging (MRI) was normal. MRI of his right shoulder showed degeneration of acromioclavicular and glenohumeral joint; subacromial impingement, subdeltoid bursitis, fraying of the supraspinatus tendon, slimming of posterior labrum. Needle electromyography (EMG) showed the presence of irregular polymorphic bursts at rest on right supraspinatus, trapezius and rhomboid muscles. While he was tapping his left fingers, amplitude and duration of potentials on these muscles decreased. When he was rolling his left shoulder or doing mental arithmetic EMG activity of the right shoulder disappeared. He was prescribed 0,125mg daily pramipexole and 225mg daily pregabalin for his medical history of restless leg syndrome and neuropatic pain of his shoulder. Antidepressant treatment and injections of Botulinum toxin A were ineffective; however, the symptoms were disappeared with clonazepam 5mg daily for a short time. But he got worse after two months, so we motivated him to have behavior modification therapy. 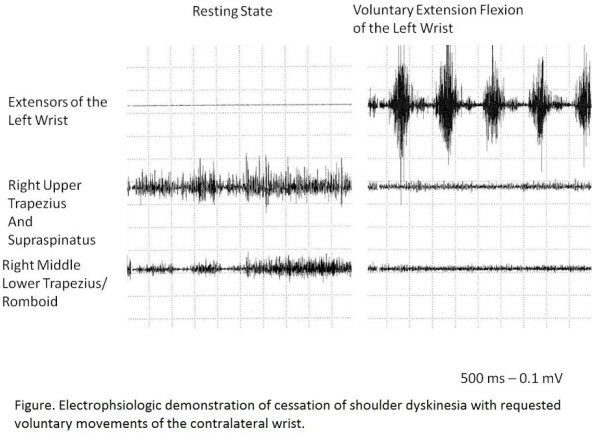
Conclusions: Similar to some reported cases, our patient was diagnosed to have functional movement disorder due to distractibility documented in physical examination and EMG, lack of explanatory laboratory findings, and atypical phenomenology.
To cite this abstract in AMA style:
S. Tezcan, M. Demirci, M.C. Akbostanci. A case with posttraumatic functional shoulder dyskinesia [abstract]. Mov Disord. 2016; 31 (suppl 2). https://www.mdsabstracts.org/abstract/a-case-with-posttraumatic-functional-shoulder-dyskinesia/. Accessed May 2, 2026.« Back to 2016 International Congress
MDS Abstracts - https://www.mdsabstracts.org/abstract/a-case-with-posttraumatic-functional-shoulder-dyskinesia/
