Category: Surgical Therapy: Parkinson's Disease
Objective: Analyze the effects of DBS on the quality of life of patients diagnosed with Parkinson’s disease.
Background: Parkinson’s disease is a neurodegenerative syndrome due to the decreased dopamine synthesis with great impact on the quality of life of the population and high worldwide prevalence. The pharmacological approach has a good response by diminishing symptoms and maintaining the individual’s well-being, however later on it is common to develop motor complications and gastrointestinal disorders. Thus, surgical treatments turn into options for invasive and efficient approaches, at later stages, such as deep brain stimulation.
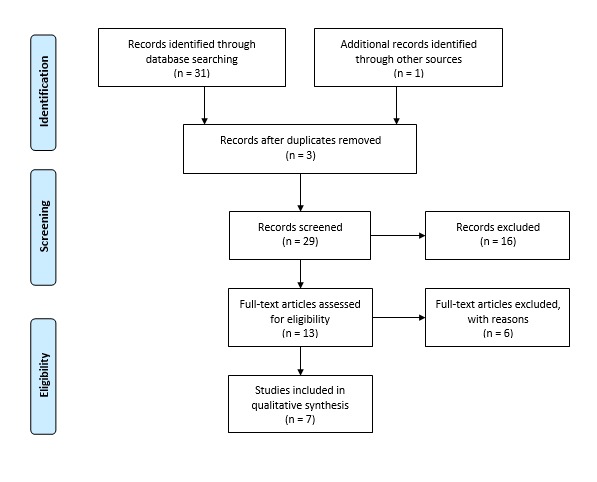
Method: A systematic review was performed based on PRISMA Statement[3]. To identify articles, the databases MEDLINE through PubMed and Science Direct, were used on March 3, 2021 and the research strategy was composed by the terms: “Parkinson disease or Idiopathic Parkinson Disease or Primary Parkinsonism” and “Deep Brain Stimulation or Brain Stimulations, Deep” and “Quality of Life of Life Quality or Health-Related Quality Of Life” and “Randomized Controlled Trial”. Randomized clinical trials were included, whose patients underwent surgery for DBS in the STN or GPi and in which the quality of life of PD patients was assessed. The exclusion criteria were studies that did not present DBS as the main intervention or that did not use the PDQ-39 to access the impact of the intervention.
Results: Among 31 studies found, in the database search, 13 met the eligibility criteria, 7 of which were eligible for qualitative analysis. 840 patients were analyzed, 450 underwent DBS and 390 under drug therapy. In general, a statistically significant improvement could be found in the assessment of quality of life in patients undergoing DBS. Weaver et al.(2012) demonstrated an improvement in quality of life in the two groups submitted to DBS after 12 and 24 months (p value statistically significant in all fields). Schuepbach et al.(2013) obtained an improvement of 26% in the DBS group P = 0.02. It is worth mentioning that Rothland et al. (2014) demonstrated that DBS is inefficient in patients with previous cognitive decline.
Conclusion: The analysis of articles revealed that PD patients undergoing DBS had significant improvements in at least one of the areas of PDQ-39. In addition, patients who already had cognitive decline before intervention did not show significant changes in QOL after treatment with DBS.
References: [1] Jr, A. L. T., & Cardoso, F. (2004). Tratamento inicial da doença de Parkinson. Revista Neurociências, 12(3), 141-146. https://doi.org/10.34024/rnc.2004.v12.8861 [2] Okun MS. Deep-brain stimulation for Parkinson’s disease. N Engl J Med. 2012 Oct 18;367(16):1529-38. doi: 10.1056/NEJMct1208070. PMID: 23075179. [3] D. Moher et al., “Preferred reporting items for systematic reviews and meta-analyses: The PRISMA statement,” PLoS Med., vol. 6, no. 7, 2009, doi: 10.1371/journal.pmed.1000097. [4] C. Daniels, P. Krack, J. Volkmann, J. Raethjen, and K. Bo, “Is Improvement in the Quality of Life After Subthalamic Nucleus Stimulation in Parkinson ’ s Disease Predictable ?,” vol. 26, no. 14, pp. 2516–2521, 2011, doi: 10.1002/mds.23907. [5] K. Witt et al., “Journal of the Neurological Sciences Negative impact of borderline global cognitive scores on quality of life after subthalamic nucleus stimulation in Parkinson ’ s disease,” J. Neurol. Sci., vol. 310, no. 1–2, pp. 261–266, 2011, doi: 10.1016/j.jns.2011.06.028. [6] WEAVER, F. M.; FOLLETT, K. A.; STERN, M.; LUO, P.; HARRIS, C. L.; HUR, K.; MARKS, W. J.; ROTHLIND, J.; SAGHER, O.; MOY, C.. Randomized trial of deep brain stimulation for Parkinson disease: thirty-six-month outcomes. Neurology, [S.L.], v. 79, n. 1, p. 55-65, 20 jun. 2012. Ovid Technologies (Wolters Kluwer Health). http://dx.doi.org/10.1212/wnl.0b013e31825dcdc1. [7] Flores Alves Dos Santos J, Tezenas du Montcel S, Gargiulo M, Behar C, Montel S, Hergueta T, et al. (2017) Tackling psychosocial maladjustment in Parkinson’s disease patients following subthalamic deep-brain stimulation: A randomised clinical trial. PLoS ONE 12(4): e0174512. [8] SCHUEPBACH, W.M.M.; RAU, J.; KNUDSEN, K.; VOLKMANN, J.; KRACK, P.; TIMMERMANN, L.; HÄLBIG, T.D.; HESEKAMP, H.; NAVARRO, S.M.; MEIER, N.. Neurostimulation for Parkinson’s Disease with Early Motor Complications. New England Journal Of Medicine, [S.L.], v. 368, n. 7, p. 610-622, 14 fev. 2013. Massachusetts Medical Society. http://dx.doi.org/10.1056/nejmoa1205158. [9] BLOMSTEDT, Patric; PERSSON, Rasmus Stenmark; HARIZ, Gun-Marie; LINDER, Jan; FREDRICKS, Anna; HÄGGSTRÖM, Björn; PHILIPSSON, Johanna; FORSGREN, Lars; HARIZ, Marwan. Deep brain stimulation in the caudal zona incerta versus best medical treatment in patients with Parkinson’s disease: a randomised blinded evaluation. Journal Of Neurology, Neurosurgery & Psychiatry, [S.L.], v. 89, n. 7, p. 710-716, 31 jan. 2018. BMJ. http://dx.doi.org/10.1136/jnnp-2017-317219. [10] Rothlind JC, York MK, Carlson K, Luo P, Marks WJ Jr, Weaver FM, Stern M. Neuropsychological changes following deep brain stimulation surgery for Parkinson’s disease: comparisons of treatment at pallidal and subthalamic targets versus best medical therapy. J Neurol Neurosurg Psychiatry. 2015 Jun;86(6):622-9. doi: 10.1136/jnnp-2014-308119. Epub 2014 Sep 2. PMID: 25185211.
To cite this abstract in AMA style:
V. Junior, I. Andrade, L. Castanheira, B. Orleans, F. da Silva, L. Magalhães. Effect of deep brain stimulation on quality of life of patients with Parkinson’s Disease [abstract]. Mov Disord. 2021; 36 (suppl 1). https://www.mdsabstracts.org/abstract/effect-of-deep-brain-stimulation-on-quality-of-life-of-patients-with-parkinsons-disease/. Accessed May 15, 2026.« Back to MDS Virtual Congress 2021
MDS Abstracts - https://www.mdsabstracts.org/abstract/effect-of-deep-brain-stimulation-on-quality-of-life-of-patients-with-parkinsons-disease/