Session Information
Date: Monday, October 8, 2018
Session Title: Parkinson's Disease: Neuroimaging And Neurophysiology
Session Time: 1:15pm-2:45pm
Location: Hall 3FG
Objective: We conducted this longitudinal study to confirm the efficacy of memantine for PDD by analyzing comparative changes in regional cerebral blood flow (rCBF) and neuropsychological tests before and after memantine administration in PDD.
Background: Memantine’s efficacy has been demonstrated in patients with moderate to severe Alzheimer’s disease (AD). However, memantine therapy is not typically used in treating Parkinson’s disease dementia (PDD), although the deviating glutamatergic pattern evidenced in neuropathological findings suggests that NMDA receptor antagonists in patients with Lewy body disorder may be effective.
Methods: We enrolled 46 patients with PDD and 18 of these patients were selected in this study. Thirty-two healthy participants were matched for age and sex with the patient group. Measures of safety assessed at specified intervals included neurologic and physical examinations, measurement of vital signs, electrocardiography, laboratory tests (hematologic tests, blood chemical values, and urinalysis), and recording of adverse events. Selected participants completed twice neuropsychological tests and perfusion brain SPECT at baseline and at 12 months after memantine therapy. The effect of memantine therapy was evaluated by statistically comparing neuropsychological test performance and regional cerebral blood flow indicated by perfusion SPECT in PDD before and 12 months after memantine therapy.
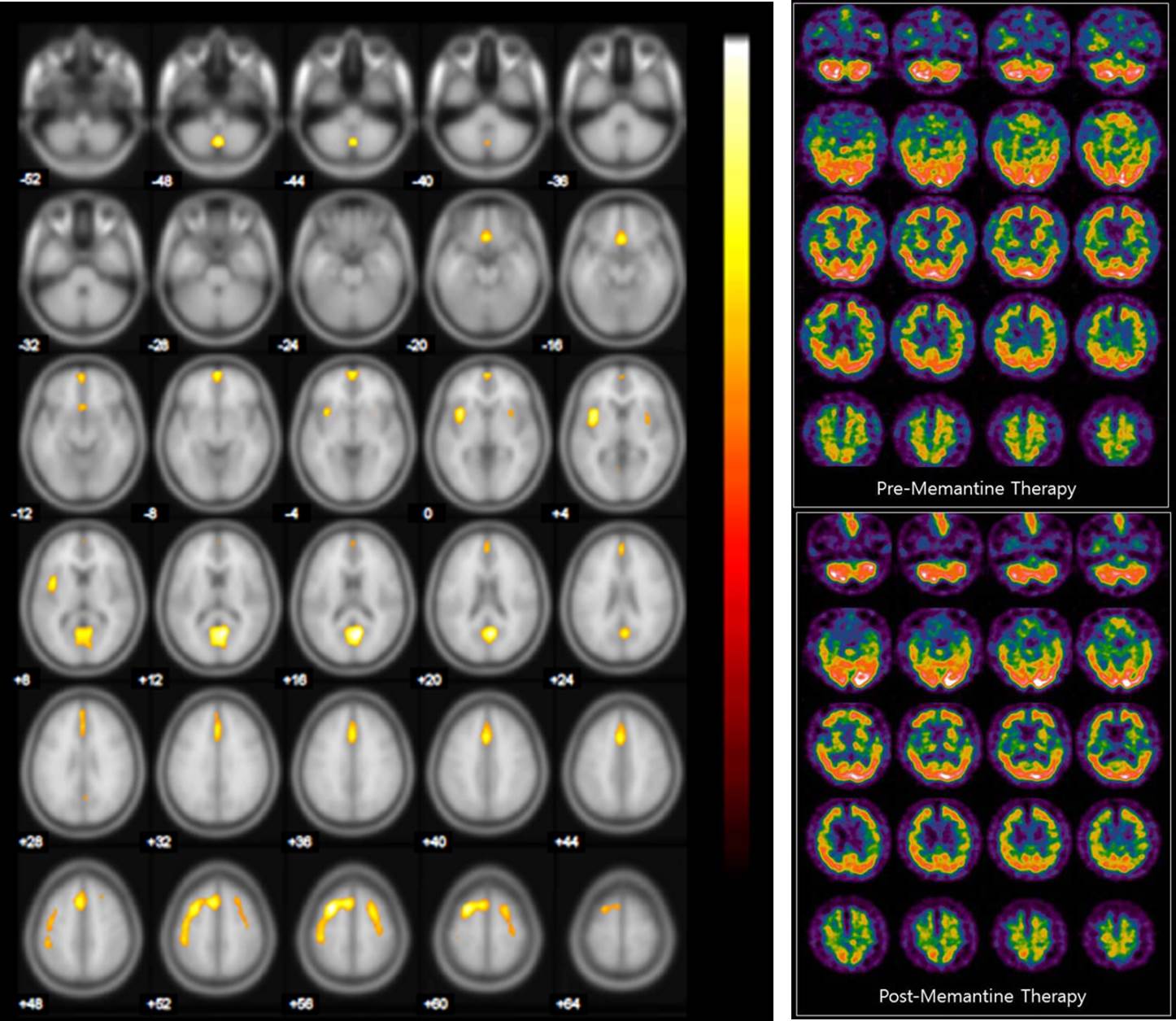
Results: A total of 18 patients (10 women) with PDD were included in the analyses. Mean age was 74.33±7.21 years. Neuropsychological tests at baseline showed a MMSE score of 15.75±5.97, CDR score of 1.56±0.98, SOB score of 9.13±4.98, GDS score of 4.75±1.04 and a total NPI score of 32.50±27.19. Neuropsychological scores at 12 months after memantine therapy showed no significant difference (MMSE=15.50±6.55, CDR=1.31±1.07, SOB=8.18±5.15, GDS=4.63±1.41 and a total NPI=34.50±39.56). Namely, there was no significant difference between initial and follow-up neuropsychological tests. SPECT analysis showed that patients with PDD at baseline had rCBF hypoperfusion bilaterally in the posterior cingulate gyri (BA 31), middle frontal gyri (BA 6), medial frontal gyri (BA 6, BA 25), insula (BA 13) and posterior cerebellum. However, there was no significant difference in rCBF observed in any regions in the PDD group at baseline compared to 12 months after memantine therapy.
Conclusions: We found that memantine appears to delay the speed of deterioration in cognitive functioning and behavioral symptoms of PDD because we observed no significant changes in rCBF or cognition 12 months after memantine therapy.
References: D. Aarsland, C. Ballard, Z. Walker, F. Bostrom, G. Alves, K. Kossakowski, I. Leroi, F. Pozo-Rodriguez, L. Minthon and E. Londos, Memantine in patients with Parkinson’s disease dementia or dementia with Lewy bodies: a double-blind, placebo-controlled, multicentre trial, Lancet Neurol 8 (2009), 613-618. S. Gauthier, Y. Wirth and H. J. Mobius, Effects of memantine on behavioural symptoms in Alzheimer’s disease patients: an analysis of the Neuropsychiatric Inventory (NPI) data of two randomised, controlled studies, Int J Geriatr Psychiatry 20 (2005), 459-464.
To cite this abstract in AMA style:
Y. Chung, I. Song, L. Lee. Effects of N-methyl-D-aspartate receptor antagonist in Parkinson’s disease with dementia [abstract]. Mov Disord. 2018; 33 (suppl 2). https://www.mdsabstracts.org/abstract/effects-of-n-methyl-d-aspartate-receptor-antagonist-in-parkinsons-disease-with-dementia/. Accessed May 23, 2026.« Back to 2018 International Congress
MDS Abstracts - https://www.mdsabstracts.org/abstract/effects-of-n-methyl-d-aspartate-receptor-antagonist-in-parkinsons-disease-with-dementia/