Category: Epidemiology
Objective: The goal of this study was to describe changes in patient-reported symptoms following initiation of standard-of-care treatment strategies in Parkinson’s disease (PD).
Background: A substantial body of evidence exists demonstrating an improvement in motor symptoms following initiation of dopaminergic therapies and deep brain stimulation (DBS) surgery, although few studies have attempted to describe the non-motor changes associated with these interventions.
Method: Data were obtained from an ongoing internet-based natural history study designed to identify modifiable variables associated with rate of PD progression. Since 2013, participants have been surveyed every six months. For this analysis, only individuals with idiopathic PD and at least 6 completed surveys during the observation period were included. Data points were compared for the single visit prior to initiating the intervention to the result immediately following.
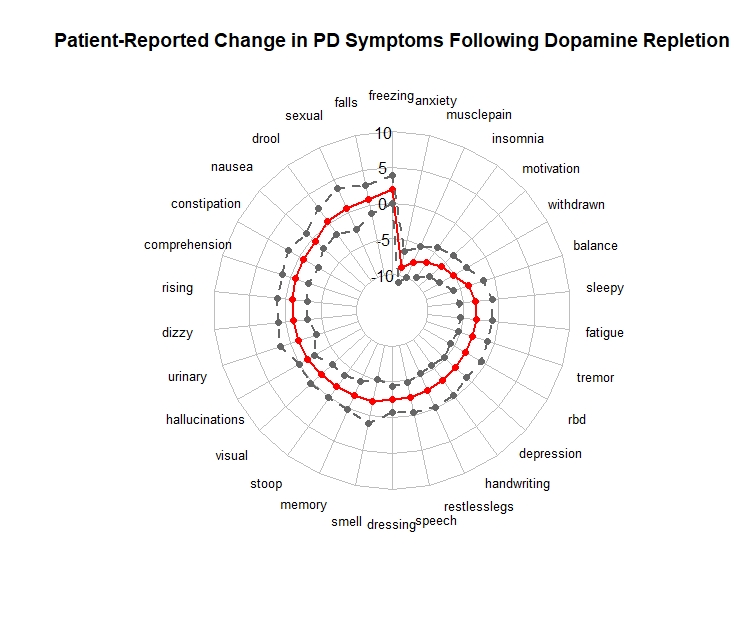
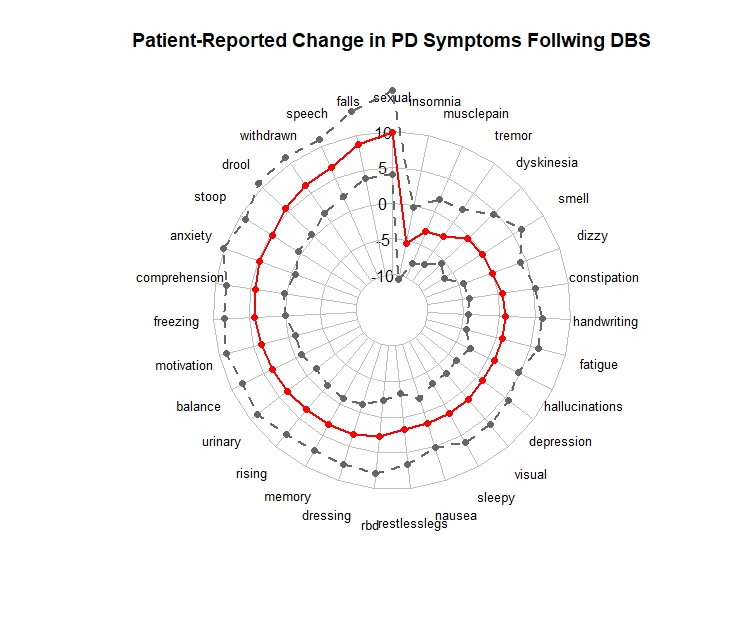
Results: During the study observation period there were 662 individuals that met the inclusion criteria, 439 of whom initiated dopaminergic therapies and 53 of whom reported having had DBS in between surveys. Patients reported improvements in motor symptoms with both interventions. Following dopamine replacement, significant improvements were observed for nonmotor symptoms anxiety, muscle pain, insomnia, motivation/ initiative, apathy and fatigue. No symptoms worsened following dopamine initiation. Following DBS, patients reported improvements in sleep, myalgia and tremor. Following DBS, there was a statistically significant worsening of sexual impairment, falls, speech, loss of interest, drooling, stooped posture, and frequent confusion.
Conclusion: In spite of widespread use of these interventions, this is the first large-scale inquiry into the patient experience following dopamine repletion and DBS. As expected, improvements in tremor were reported following both interventions. Unexpectedly, individuals reported significant nonmotor symptom improvements following dopamine repletion and a worsening of nonmotor symptoms following DBS. Whereas dopamine become effective over weeks, it can take months to optimize settings following DBS; it is possible DBS outcomes might improve over subsequent surveys. Further evaluation of the effects of DBS on short- and long-term nonmotor symptoms is warranted.
To cite this abstract in AMA style:
L. Mischley, C. Weaver, J. Farahnik, Y. Chien. Patient-Reported Impact of Standard-of-Care: Change in Symptoms Following Dopamine Initiation and Deep Brain Stimulation [abstract]. Mov Disord. 2021; 36 (suppl 1). https://www.mdsabstracts.org/abstract/patient-reported-impact-of-standard-of-care-change-in-symptoms-following-dopamine-initiation-and-deep-brain-stimulation/. Accessed May 3, 2026.« Back to MDS Virtual Congress 2021
MDS Abstracts - https://www.mdsabstracts.org/abstract/patient-reported-impact-of-standard-of-care-change-in-symptoms-following-dopamine-initiation-and-deep-brain-stimulation/