Objective: The purpose of this study was to examine clinical utility of the 20-item Noise Pareidolia Task (NPT20) in Parkinson’s disease (PD), as indicated by sensitivity and specificity to complex visual hallucinations (VH) and convergent validity with related visuospatial function measures.
Background: Complex VH are a common and often troublesome complication of PD. Association with visuospatial impairment[1] and abnormal metabolic function[2] implicate posterior cortical involvement. Recent studies have demonstrated relevance of pareidolia phenomenon, “false perception of faces”, to VH in PD and Lewy body dementia (LBD). An abbreviated test, the NPT20, was validated in LBD [3], but clinical utility in PD has not been established.
Method: This retrospective chart review included 46 consecutive PD patients who completed NPT20 during clinical neuropsychological evaluation. Persistent complex VH was queried during clinical interview and noted as present or absent. Cognitive diagnosis followed MDS Task Force Level II diagnostic criteria.
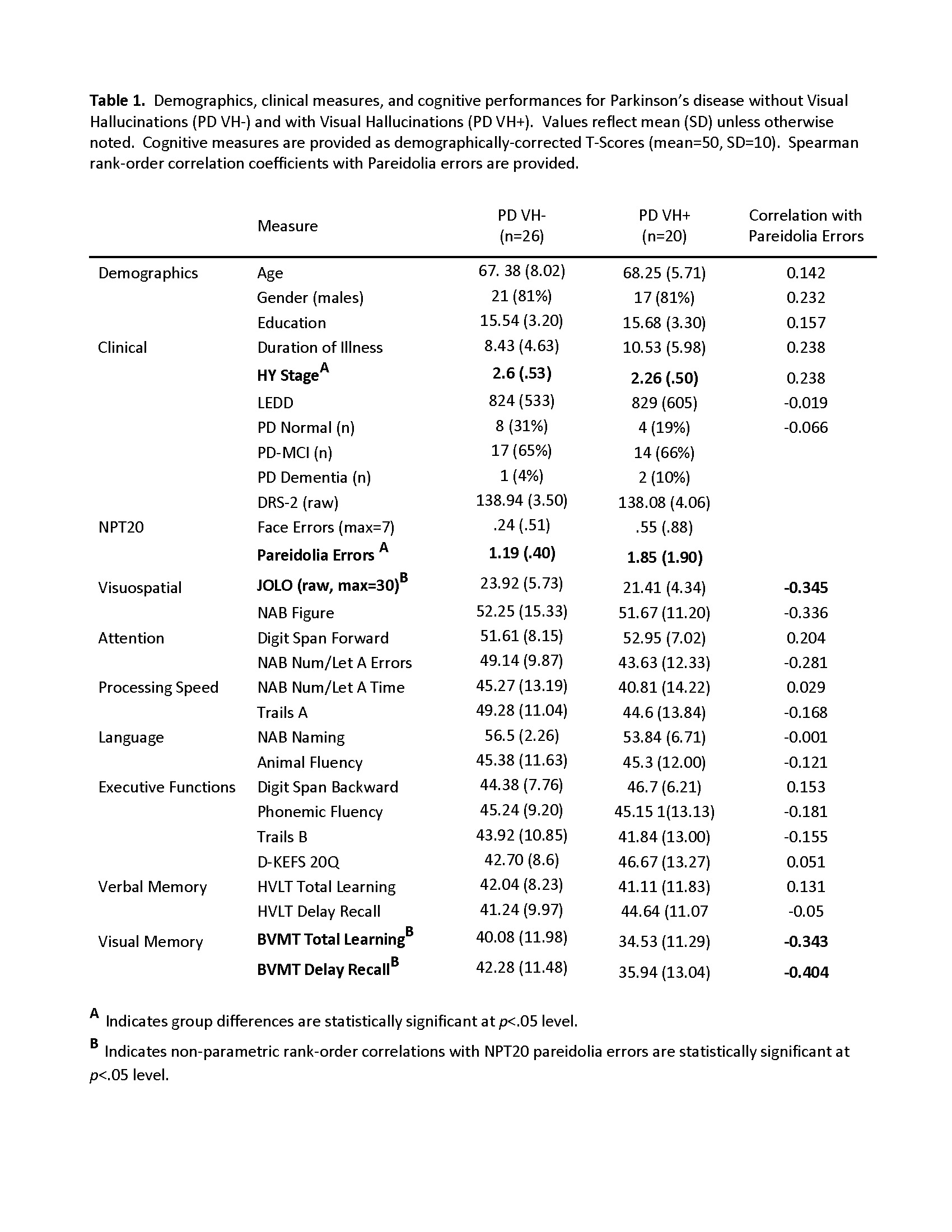
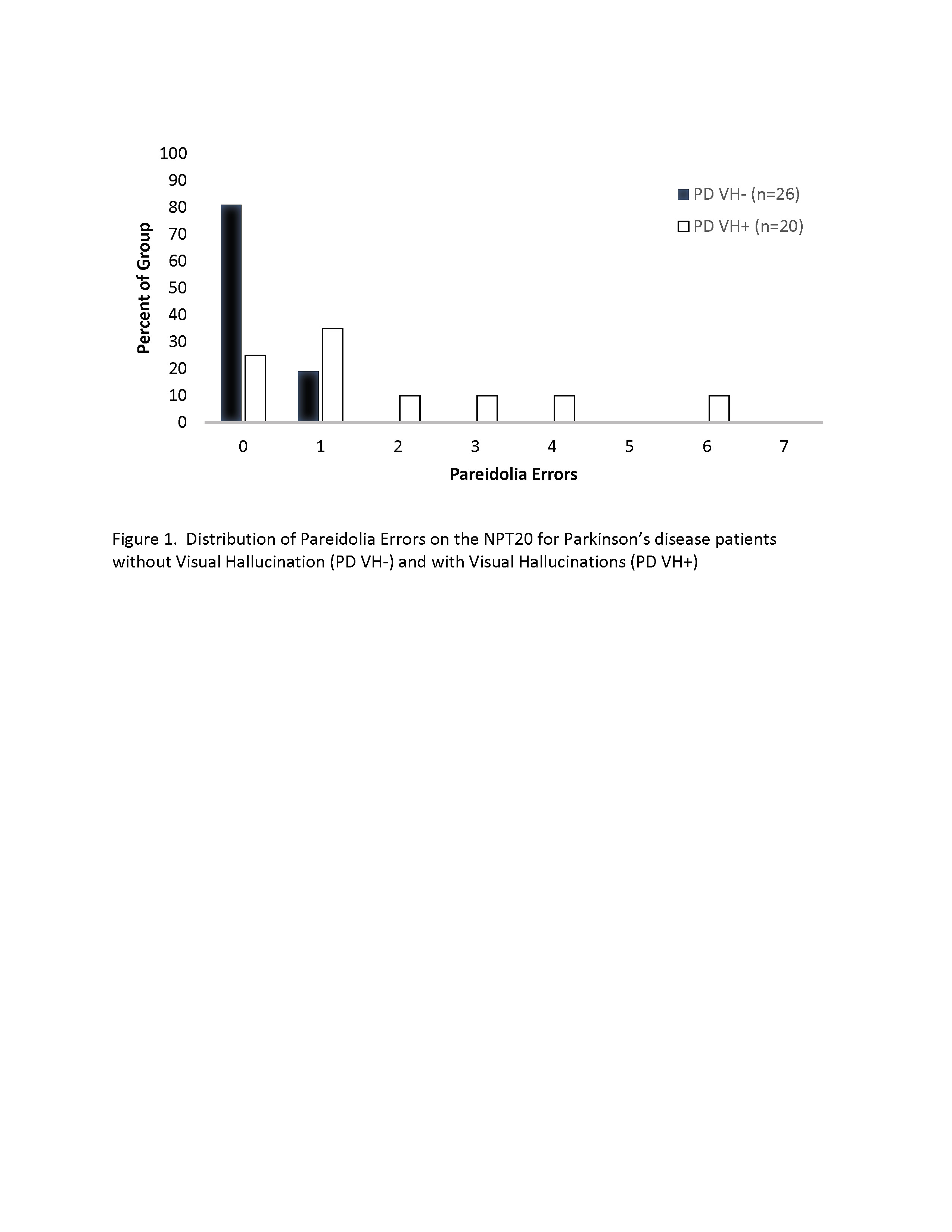
Results: About half the sample (43%) reported complex VH. VH was associated with greater disease severity, HY Stage=2.6 vs 2.26, p=.04, but no other clinical or demographic factor [Table1]. PD patients reporting VH made significantly more false-positive pareidolia errors on the NPT20 (p<.0001). Statistically significant group differences were not seen on any other cognitive measure, and cognitive status was not associated with pareidolia errors. Across groups, NPT20 evinced moderate correlations with visual perception (JOLO) and visual memory (BVMT). Distribution of pareidolia errors by group are shown in Figure 1 [Figure1]. A cut-off of 2 errors yielded 40% sensitivity and 100% specificity to VH; cut-off of 1 error provided 75% sensitivity and 81% specificity.
Conclusion: The NPT20 is a brief objective assessment tool that appears uniquely sensitive to visuoperceptual disturbances underlying complex VH in PD. These findings are consistent with prior studies in LBD. Future studies will examine association of NPT20 with delusions in PD, and identify factors driving VH in PD who do not make pareidolia errors.
References: [1] Specketer K, Zabetian CP, Edwards KL, Tian L, Quinn JF, Peterson-Hiller AL, Chung KA, Hu SC, Montine TJ, Cholerton BA. Visuospatial functioning is associated with sleep disturbance and hallucinations in nondemented patients with Parkinson’s disease. J Clin Exp Neuropsychol. 2019 Oct;41(8):803-813. PMID: 31177941; PMCID: PMC6681669.
[2] Uchiyama M, Nishio Y, Yokoi K, Hosokai Y, Takeda A, Mori E. Pareidolia in Parkinson’s disease without dementia: A positron emission tomography study. Parkinsonism Relat Disord. 2015 Jun;21(6):603-9. PMID: 25864093.
[3] Galvin JE, Chrisphonte S, Cohen I, Greenfield KK, Kleiman MJ, Moore C, Riccio ML, Rosenfeld A, Shkolnik N, Walker M, Chang LC, Tolea MI. Characterization of dementia with Lewy bodies (DLB) and mild cognitive impairment using the Lewy body dementia module (LBD-MOD). Alzheimers Dement. 2021 Oct;17(10):1675-1686. PMID: 33793069; PMCID: PMC8484363.
To cite this abstract in AMA style:
T. Turner, F. Rodriguez-Porcel. The 20-item Noise Pareidolia Task is uniquely sensitive to Visual Hallucinations in Parkinson’s Disease [abstract]. Mov Disord. 2022; 37 (suppl 2). https://www.mdsabstracts.org/abstract/the-20-item-noise-pareidolia-task-is-uniquely-sensitive-to-visual-hallucinations-in-parkinsons-disease/. Accessed April 16, 2026.« Back to 2022 International Congress
MDS Abstracts - https://www.mdsabstracts.org/abstract/the-20-item-noise-pareidolia-task-is-uniquely-sensitive-to-visual-hallucinations-in-parkinsons-disease/