Session Information
Date: Monday, October 8, 2018
Session Title: Parkinson's Disease: Cognition
Session Time: 1:15pm-2:45pm
Location: Hall 3FG
Objective: To investigate the contribution of amyloid depositions to cognitive deficits in the early phase of Parkinson’s disease (PD).
Background: Involvement of amyloid deposits is still poorly defined particularly in the early stages of the disease.
Methods: We analyzed data of a multicenter cohort of 48 PD patients from the Parkinson’s Progression Marker Initiative who underwent [18F]florbetaben positron emission tomography (for the quantitative assessment of amyloid), clinical and cognitive examination. We evaluated global cognition using Montreal Cognitive Assessment (MoCA), memory with Hopkins Verbal Learning Test-Revised (HVLT-R), visuospatial function with Benton Judgment of Line Orientation (JLO), attentive and executive functions with Symbol-Digit Modalities Test (SDMT), working memory with Letter-Number Sequencing (LNS) and language abilities with the semantic fluency test. All the tests were corrected according to the published norms. A composite standard uptake value ratio (SUVR) for each subject was established by calculating the mean SUVRs from regions of interest, typically associated with increased uptake (Rowe et al. 2008). Composite SUVR values > 1.43 were considered amyloid positive (Aβ+), indicating presence of amyloid in the range expected for Alzheimer’s disease (Bullich et al., 2017). We defined PD Aβ+ and Aβ- according to this SUVR cut-off. Due to the non-normal distribution of the sample, descriptive and non-parametric statistics were conducted.
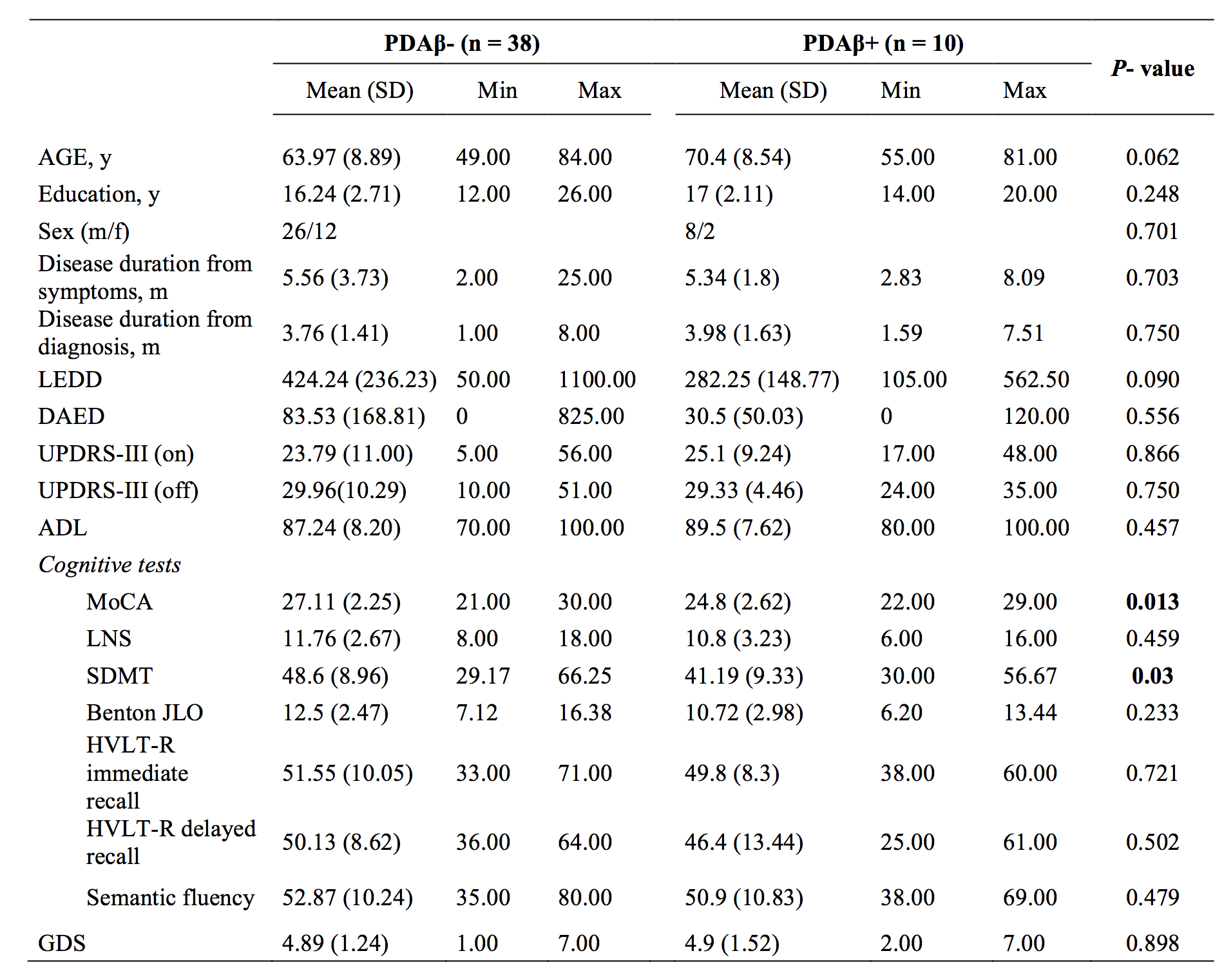
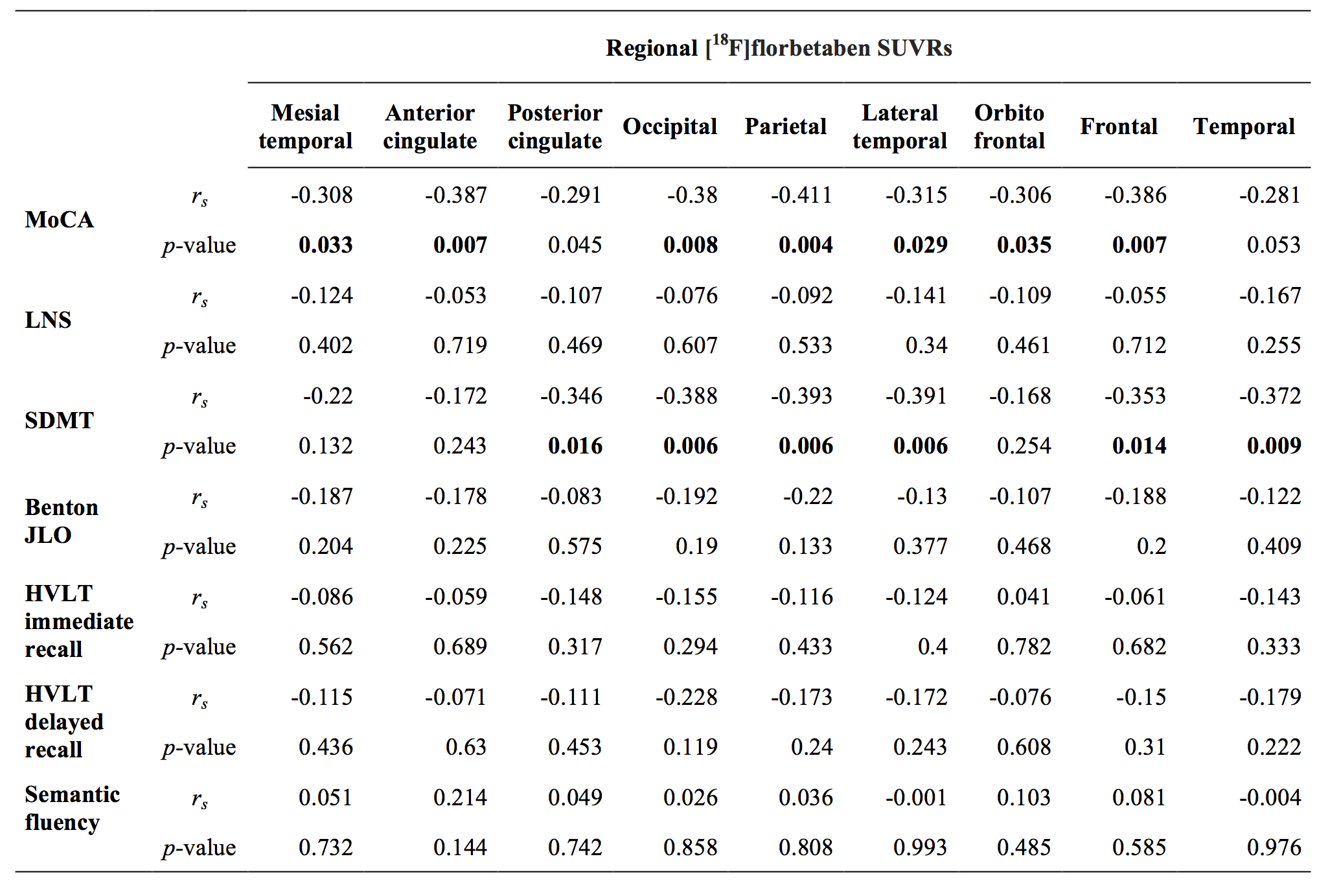
Results: We observed that 21% (n=10) of early-PD patients were amyloid-positive. Between-group comparison showed significant lower MoCA and SDMT scores in PDAβ+ compared to Aβ- group [table1]. We found an inverse correlation between amyloid tracer uptake in widespread cortical regions and these two tests [table2].
Conclusions: Widespread cortical amyloid deposition can be observed in early stage PD patients and this is associated with greater cognitive impairment as compared to amyloid negative group. Brain amyloid accumulation contributes to cognitive manifestations in PD.
References: Bullich S, Villemagne VL, Catafau AM, Jovalekic A, Koglin N, Rowe CC, De Santi S. (2017) Optimal reference region to measure longitudinal amyloid-β change with 18F-florbetaben PET. Journal of Nuclear Medicine 1;58(8):1300-6. Rowe CC, Ackerman U, Browne W, Mulligan R, Pike KL, O’Keefe G, Tochon-Danguy H, Chan G, Berlangieri SU, Jones G, Dickinson-Rowe KL, Kung HP, Zhang W, Kung MP, Skovronsky D, Dyrks T, Holl G, Krause S, Friebe M, Lehman L, Lindemann S, Dinkelborg LM, Masters CL, Villemagne VL (2008) Imaging of amyloid β in Alzheimer’s disease with 18F-BAY94-9172, a novel PET tracer: proof of mechanism. Lancet Neurol 7:129–135.
To cite this abstract in AMA style:
E. Fiorenzato, R. Biundo, D. Cecchin, AC. Frigo, L. Weis, J. Kim, A. Strafella, A. Antonini. Amyloid deposition affects cognitive manifestations in Parkinson’s disease: The PPMI dataset [abstract]. Mov Disord. 2018; 33 (suppl 2). https://www.mdsabstracts.org/abstract/amyloid-deposition-affects-cognitive-manifestations-in-parkinsons-disease-the-ppmi-dataset/. Accessed June 10, 2026.« Back to 2018 International Congress
MDS Abstracts - https://www.mdsabstracts.org/abstract/amyloid-deposition-affects-cognitive-manifestations-in-parkinsons-disease-the-ppmi-dataset/